Problems with Latching On or Sucking
It's common in the first days of life for a baby to have trouble latching on or maintaining sucking at the breast. If this problem doesn't go away, more help is needed. A baby must be able to remove enough milk from the breast through correct latch and sucking to gain weight. This milk removal then tells the breasts to increase or maintain milk production. If the baby doesn't get enough milk, they will have poor weight gain. Poor milk removal from the breast can also affect milk supply.
Many things can affect a baby's ability to suck and remove milk. Factors such as prematurity, jaundice, infection, heart disease, a mother's medicines, and many others can affect a baby's ability to stay alert or coordinate the suck-swallow-breathe actions. Other mechanical issues that may play a role include tongue-tie or a cleft lip or cleft palate. These might directly interfere with a baby's ability to use the structures in the mouth for effective sucking.
Sometimes the cause is obvious. Often it's not. But it's important to recognize the signs that a baby can't effectively remove milk during breastfeeding. Then the baby's healthcare provider can make sure that there are no health or mechanical issues affecting feeding. And steps can be taken to fix the problem.
Below are some signs of ineffective sucking.
The baby who normally:
-
Doesn't wake on their own to cue for feedings
-
Cues to feed fewer than 8 times in a 24-hour period
-
Cues to feed 14 or more times in a 24-hour period
-
Latches on and then lets go of the breast repeatedly
-
Pushes away or resists latch-on
-
Falls asleep within 5 minutes of latch-on or after sucking for only 2 or 3 minutes
-
Doesn't suck almost continuously for the first 7 to 10 minutes of a feeding
-
Nurses on one side for longer than 30 to 40 minutes
-
Feeds for more than 45 minutes without acting satisfied or full after a meal
-
Produces fewer than 3 to 4 stools in 24 hours (3 to 4 stools per day is normal for a baby who is more than 1 week old and younger than 1 month)
-
Seems gassy or produces green, frothy stools after the first week
-
Produces fewer than 6 wet diapers in 24 hours (a baby produces 6 wet diapers a day by the end of the first week)
-
Has trouble taking milk by other feeding methods
The mother who:
-
Always has sore or bruised nipples or areola
-
Gets red, scraped, or cracked nipples
-
Often has misshapen nipples after feedings (such as creased or flattened)
-
Rarely or never notices breast fullness before nursing and breast softening after nursing. This is even more likely if there are several hours between feedings.
-
Has more than 1 episode of plugged milk ducts or mastitis
How you can help with the breastfeeding process
When a problem with latch-on or sucking continues beyond the first few days after birth, it can be discouraging. Most babies will learn to breastfeed effectively if they are given time. But it's important to work with the baby's healthcare provider and a certified lactation consultant (IBCLC) if a baby has trouble latching or sucking. Until the issue is fixed, there are a few things you can do. These will help breastfeeding progress while you make sure your baby is getting enough to eat. Always talk with your baby's healthcare provider for more information:
-
Wake the baby to breastfeed every 2 to 3 hours if they are sleepy and still have not mastered feeding cues.
-
Your baby likely will do better for some feedings. Don't be discouraged if they are too sleepy. Or if they seem to forget from feeding to feeding.
-
Some feedings will last longer than others. Your baby may need time to get going at the breast for some feeds.
-
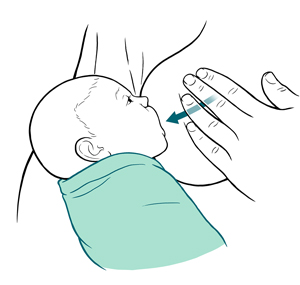
Massage your breast toward the nipple (or use one hand to gently squeeze the breast) to send milk into the baby's mouth when they are nursing. This is also helpful when your baby begins to fall asleep at the breast too soon after starting to feed. If your baby is consistently sleepy at the breast, talk with your baby's healthcare provider to learn how to offer more calories.
-
Chart the number, amount, and color of urine and stools for wet and dirty diapers on a daily record until latching and sucking is better.
-
Use a correctly fitted, hospital-grade, electric breast pump to be sure all milk is removed. Many women will express milk by pumping for a few minutes after breastfeeding. How long you will need to keep pumping depends on how quickly your baby learns to breastfeed effectively. It also depends on how much milk your baby needs to grow beyond what you are providing with breastfeeding.
-
Weigh the baby often. Or record a test weight before and after a feeding. This is best done at the office of a lactation consultant or the baby's healthcare provider with a medical-grade breastfeeding scale.
-
Certain breastfeeding devices or alternative feeding methods may encourage effective sucking. Or they may give your baby added nutrition while they are learning to breastfeed. A certain device may be good for your situation. But every device also has disadvantages. To prevent problems, any breastfeeding device should be used with the guidance of a certified lactation consultant (IBCLC) or healthcare provider with advanced knowledge of breastfeeding. Devices that may be helpful in certain situations include:
-
Nipple shield. This thin silicone device is centered over the nipple and areola. It encourages a better latch, more effective sucking pattern, and better milk intake during breastfeeding for certain babies.
-
Feeding tube system. A feeding tube system may be taped to the breast or your finger. It lets the baby get additional milk through the tube when they suck. To do this, a thin feeding tube is attached to a syringe and taped to your breast or your finger (finger feeding). Then you or a helper can gently press the plunger. This sends a few drops of milk into the baby's mouth if they forget to suck. Commercial feeding tube systems are also available.
-
Alternative feeding methods. There are also other alternative feeding methods. These will make sure that your baby gets enough food. But they are less likely to interfere with long-term breastfeeding. These include cup feeding, syringe feeding, spoon feeding, or (eye) dropper feeding. If using a bottle, bottle nipples with a slower flow rate are often preferred.
-
If any structural change in your baby's mouth is found, work with the healthcare provider to correct or treat it. Depending on the type of variation, this may include anything from mouth exercises to surgical treatment.
Other ways to help a baby with ineffective sucking
Other hints for the baby include:
-
Skin-to-skin contact seems to help a lot of babies with nursing. This also helps you maintain milk production.
-
When a baby has the basic idea of effective sucking but can't seem to do it consistently, try pumping one breast while breastfeeding your baby on the other.

-
You may want to limit the time of each breastfeeding session if you or your baby get too frustrated. Or if the feedings take more than 40 to 45 minutes. This will give you more time to pump and remove milk effectively. You may also find it's easier to be patient through the learning process. You can always express milk and give it by an alternative feeding method.
-
You may want to let the baby's father or other family members and friends handle alternative feedings. That way, you won't get overwhelmed. This frees you to focus on breastfeeding, maintain pumping sessions, and enjoy cuddling skin-to-skin with your baby.
-
Don't throw away any breastfeeding device or an alternative feeding method because you did not like it or it did not work when first suggested. The device or method that did not help one day may work great the next.
-
Once your baby is growing and developing correctly and their nutritive sucking ability is improving, ask your baby's healthcare provider when you can stop waking them for feedings and begin to wait to see if they will demonstrate feeding cues. You will also want to know when it's safe to start decreasing supplementary feedings, if they are needed.
-
Keep thinking positively. It's normal to get frustrated and think your baby will never learn to breastfeed effectively. It's normal if some days seem an eternity of breastfeeding practice, alternative feedings, and breast pumping sessions. It's normal for your confidence to rise and fall. Try to keep perspective by having a sense of humor. Think about how far your baby and you have come since their birth, not how far you still may have to go.
-
Get support. Stay in touch with the baby's healthcare provider and a certified lactation consultant. But also contact a breastfeeding support organization. They will have lots of information. And they'll give you moral support whenever you need it.
Online Medical Reviewer:
Angela Morrison LPN IBCLC
Online Medical Reviewer:
Heather M Trevino BSN RNC
Online Medical Reviewer:
Tennille Dozier RN BSN RDMS
Date Last Reviewed:
1/1/2024
© 2000-2025 The StayWell Company, LLC. All rights reserved. This information is not intended as a substitute for professional medical care. Always follow your healthcare professional's instructions.