Pinched Nerve
What is a pinched nerve?
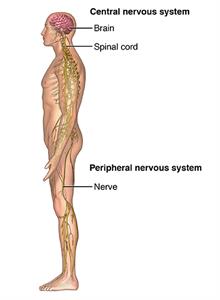
Your spine is made of many bones called vertebrae. Your spinal cord runs downward through a canal in the center of these bones. Nerve roots branch off the cord and go between each vertebra. When problems affect these nerve roots, the condition is called radiculopathy, or more commonly, a pinched nerve.
This problem is most likely to occur in your low back (lumbar radiculopathy), but it can also affect your neck (cervical radiculopathy) or other parts of your spine. Nerves can also get pinched by tendons and ligaments in your arms or legs. This is called mononeuropathy.
What causes a pinched nerve?
One cause of a pinched nerve is a herniated disk. Soft disks act as cushions between your vertebrae. Sometimes, these disks slip out of place or become damaged and press on nerves. This is also called a slipped disk.
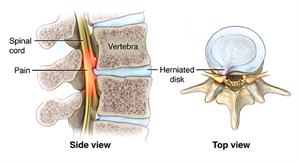
As people age, it's common for the disks to become shorter and the vertebrae to get closer together. Bone growths called spurs could also press on the nerve roots. But many people age 50 and older have damaged disks and pinched nerves with no symptoms.
What are the symptoms of a pinched nerve?
Symptoms of a pinched nerve in the low back include:
-
A sharp pain in the back that may travel all the way to your foot
-
Pain that may become worse with certain activities like sitting or coughing
-
Numbness of the skin in areas of the leg or foot
-
Weakness in the leg
Symptoms of pinched nerve in the neck include:
How is a pinched nerve diagnosed?
You will first have a physical exam. Your healthcare provider will test your reflexes and your ability to sense things. They will also check your ability to move your muscles. You may need to lie on your back and lift your leg while holding it straight or do other movements. If you have pain with certain movements, it may help with the diagnosis.
You may also need:
-
Imaging tests. You may have an X-ray, CT scan, or MRI scan. These tests let your healthcare provider see the structures in your neck or back. Your healthcare provider may also inject a contrast material (a dye) into your spinal canal to help show the problem area.
-
Nerve conduction tests and electromyography (EMG). These check nerve function.
How is a pinched nerve treated?
In many cases, these simple steps may treat your symptoms:
-
Medicine such as nonsteroidal anti-inflammatory drugs (NSAIDs), narcotic medicines for more severe pain, and muscle relaxants
-
Losing weight, if needed, with diet and exercise
-
Physical therapy or a supervised home exercise program
-
For a pinched nerve in the neck, wearing a soft collar around your neck for short amounts of time
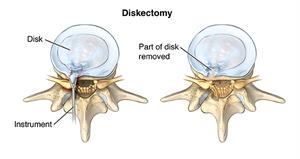
Some people need more advanced treatments. Your healthcare provider might suggest injections of steroid medicine in the area where a disk is herniated. Some people might benefit from surgery. During a surgical procedure called a discectomy, the surgeon removes all or part of the disk that is pressing on a nerve root. Along with this procedure, the surgeon may need to remove parts of some vertebrae or fuse vertebrae together.
 |
| PNerv_20140108_v0_001 |
What can I do to prevent a pinched nerve?
Staying physically fit may reduce your risk of having a pinched nerve. Using good posture at work and in your leisure time, such as lifting heavy objects properly, may also help prevent this condition. Correct placement of your computer keyboard and frequent breaks can help reduce the risk of a pinched nerve in the wrist, such as carpal tunnel syndrome. If you sit at work for long periods, consider getting up and walking around regularly. A healthy lifestyle that includes not smoking, regular exercise (including muscle strengthening and stretching exercises), and eating well may also reduce the risk for a pinched nerve.
Living with a pinched nerve
Medicines like nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroids, or stronger pain medicines help reduce nerve swelling and relieve pain. Corticosteroids may also be given as an injection, which will also reduce inflammation and pain allowing the nerve to heal. Wearing a wrist splint at night can help symptoms of carpal tunnel syndrome.
Losing weight, if needed, will help relieve pressure on the joints. Physical therapy may use specialized exercises to strengthen and stretch the back or neck muscles. A physical therapist may suggest wearing a soft collar or using traction to help the neck muscles rest and heal. Your healthcare provider may suggest a home exercise program that you can do on a routine basis. These measures also relieve pressure on the nerve.
Your healthcare provider may be able to suggest self-care steps to help prevent or treat a pinched nerve.
When should I call my healthcare provider?
Call your healthcare provider right away or go to the emergency room if you have:
-
Sudden onset of numbness, weakness, or paralysis of an arm or leg that does not go away
-
Loss of bladder or bowel control
-
Loss of sensation in your genital or anal regions
These could be signs of a serious condition that needs treatment right away.
Key points about a pinched nerve
-
A pinched nerve (radiculopathy) is caused by a disk or bone in the spine that presses on a nerve root coming out of the spinal cord.
-
Symptoms can include pain, numbness, or weakness in an arm or leg.
-
A pinched nerve can often be helped with medicines, physical therapy, weight loss, and rest, although more involved treatments might be needed in some cases.
-
Prevention and symptom reduction includes weight management, regular activity, healthy eating, and muscle strengthening exercises.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
-
Know the reason for your visit and what you want to happen.
-
Before your visit, write down questions you want answered.
-
Bring someone with you to help you ask questions and remember what your provider tells you.
-
At the visit, write down the name of a new diagnosis, and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you.
-
Know why a new medicine or treatment is prescribed, and how it will help you. Also know what the side effects are and when they should be reported.
-
Ask if your condition can be treated in other ways.
-
Know why a test or procedure is recommended and what the results could mean.
-
Know what to expect if you do not take the medicine or have the test or procedure.
-
If you have a follow-up appointment, write down the date, time, and purpose for that visit.
-
Know how you can contact your provider if you have questions.