Huntington Disease
What is Huntington disease?
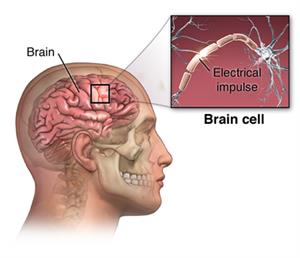
Huntington disease is a brain disorder in which brain cells, or neurons, in certain areas of your brain start to break down. As the neurons degenerate, the disease can lead to emotional disturbances, loss of intellectual abilities, and uncontrolled movements.
 |
| ANerv_20140205_v1_001 |
Huntington disease has 2 subtypes:
-
Adult-onset Huntington disease. This is the most common form of Huntington disease. People typically develop the symptoms in their mid-30s and 40s.
-
Early-onset Huntington disease. In rare instances, children or adolescents will develop the disease. Children with the disease tend to experience abrupt difficulties with schoolwork and often have symptoms that are quite similar to Parkinson disease.
What causes Huntington disease?
Huntington disease is a genetic disorder. It is passed on from parents to children. If a parent has Huntington disease, the child has a 50% chance of developing it. If the child doesn’t develop the disease, he or she won’t pass it along to his or her children. For 1% to 3% of people with Huntington disease, no family history of the disorder is ever identified.
What are the symptoms of Huntington disease?
As the disease progresses, the following symptoms become more common:
-
Trouble feeding oneself
-
Difficulty swallowing
-
Strange and uncontrolled movements that are either slow or wild and jerking (chorea)
-
Loss of memory and judgment
-
Changes in speech
-
Personality changes
-
Disorientation and confusion
-
Hallucinations, paranoia, and psychosis
In children, the symptoms often include Parkinson disease‒like features such as:
-
Slow movements
-
Rigidity
-
Tremors
How is Huntington disease diagnosed?
Because many of these symptoms can be caused by other diseases, a detailed physical and neurological exam is usually needed. Not surprisingly, a family history of the disorder is often the biggest clue that you may have Huntington disease.
Special blood tests can help your healthcare provider determine your likelihood of developing Huntington disease. A computed tomography (CT) scan of the head can evaluate the scope and scale of brain cell damage and loss of brain tissue. A magnetic resonance imaging (MRI) scan or a positron emission tomography (PET) scan may also be used.
What are the risk factors for Huntington disease?
If you have the Huntington disease gene, you will develop the disease at some point during your life. The age of onset of Huntington disease varies greatly from person to person, but most people develop it in their 30s or 40s.
Huntington disease is a rare disorder. More than 15,000 Americans currently have the disease, but many more are at risk of developing it.
How is Huntington disease treated?
You can’t cure or slow the progression of Huntington disease, but health care providers can offer medications to help with certain symptoms.
Drugs like haloperidol, tetrabenazine, and amantadine are especially helpful for controlling the unusual movements caused by Huntington disease. Haloperidol and tetrabenazine can also help offset hallucinations and delusional thoughts. Depression and suicide are common among those with Huntington disease. Antidepressants and antianxiety medications may be prescribed to treat these symptoms.
Living with Huntington disease
As Huntington disease progresses, you will need constant assistance and supervision because of the debilitating nature of the disease. People usually die from the disease within 15 to 20 years of developing symptoms.
If you have been diagnosed with, or are at risk for Huntington disease, it is critical to maintain your physical fitness as best you can. People who exercise regularly and stay active tend to do better than those who don’t.
A number of studies are currently under way to examine possible therapies for Huntington disease. Talk with your health care provider about whether any of these therapies may be helpful to you or a loved one with the disorder.
When should I call my healthcare provider?
If you have Huntington disease, it is important to closely monitor you condition, and contact your healthcare provider if you notice any of the following symptoms:
-
Increasing difficulty with motor tasks such as walking
-
Trouble swallowing
-
Mood changes, such as increasing symptoms of depression or feelings of suicide
Key points
-
Huntington disease is a genetic brain disorder.
-
There is no cure at this time.
-
The goal of treatment is to manage your symptoms so that you can function as long as possible.
-
If you have Huntington disease, your child has a 50% chance of developing the disease.
-
Huntington disease affects your emotional, physical, and intellectual abilities.
-
As the disease progresses, you will need additional assistance and supervision; eventually you will need help 24 hours a day.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
-
Know the reason for your visit and what you want to happen.
-
Before your visit, write down questions you want answered.
-
Bring someone with you to help you ask questions and remember what your provider tells you.
-
At the visit, write down the name of a new diagnosis, and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you.
-
Know why a new medicine or treatment is prescribed, and how it will help you. Also know what the side effects are.
-
Ask if your condition can be treated in other ways.
-
Know why a test or procedure is recommended and what the results could mean.
-
Know what to expect if you do not take the medicine or have the test or procedure.
-
If you have a follow-up appointment, write down the date, time, and purpose for that visit.
-
Know how you can contact your provider if you have questions.